The field of orthopedic surgery has undergone a massive transformation over the last few decades. Among the most significant advancements in trauma care is the evolution of internal fixation techniques for long bone fractures. When a person suffers a severe break in the femur (thigh bone), tibia (shin bone), or humerus (upper arm bone), the primary goal of the surgeon is to restore alignment and allow for early movement. This is where Interlocking Nail Systems have become the gold standard of modern treatment.
In this guide, we will explore what these systems are, how they function, and why they have revolutionized the way surgeons approach complex bone injuries.
What are Interlocking Nail Systems?
An interlocking nail is a sophisticated metal rod—typically made of titanium or high-grade stainless steel—that is inserted into the medullary canal (the hollow center) of a long bone. While intramedullary (IM) nailing has been used since the mid-20th century, the “interlocking” component changed everything.
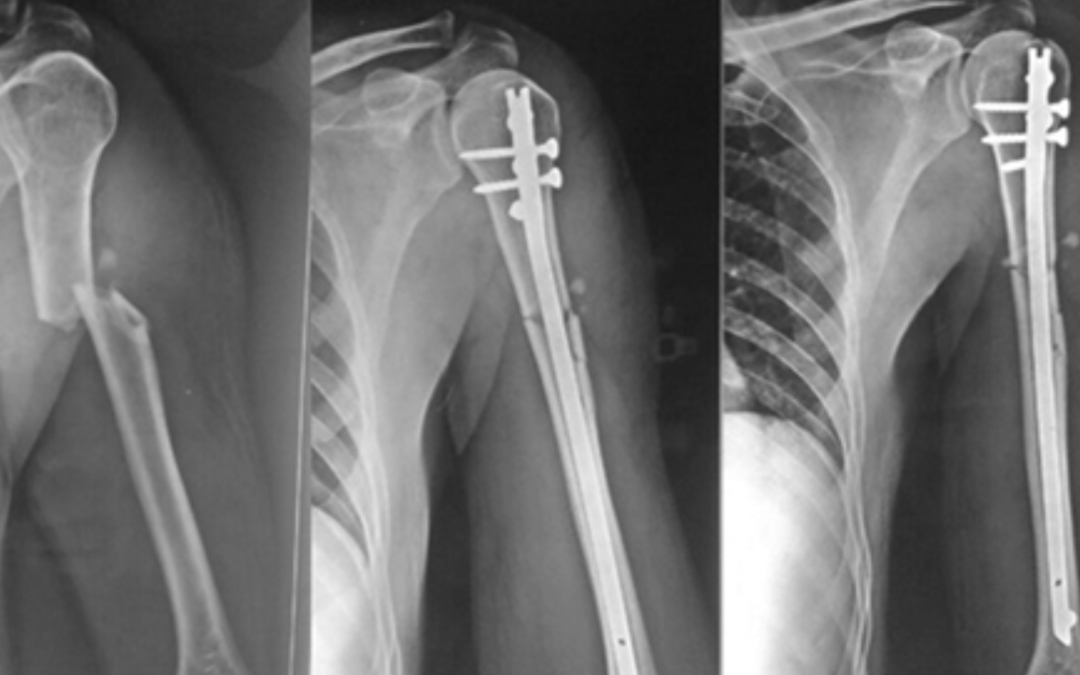
Traditional nails relied on a tight friction fit within the bone to stay in place. However, if a fracture was unstable or near the end of the bone, the nail could slide or rotate. Interlocking Nail Systems solve this by using transverse locking screws that pass through the bone and the nail at both the top (proximal) and bottom (distal) ends. This “locks” the nail into the bone, preventing the fracture from shortening or rotating, and providing unparalleled mechanical stability.
The Biomechanics of Internal Fixation
To understand why Interlocking Nail Systems are so effective, one must understand the “load-sharing” principle. Unlike bone plates, which are fixed to the outer surface of the bone (load-bearing), an intramedullary nail sits in the center of the bone.
Because the nail is positioned along the bone’s natural longitudinal axis, it shares the weight-bearing forces with the bone itself. This distribution of stress reduces the risk of hardware failure and encourages the bone to heal more naturally. The locking screws ensure that even if the bone is shattered into multiple fragments, the overall length and alignment of the limb are maintained throughout the healing process.
Key Advantages of Modern Interlocking Nails
The adoption of these systems has led to significantly better outcomes for patients globally. Here are the primary benefits:
1. Minimal Soft Tissue Disruption
Old-fashioned surgery often required large incisions to expose the entire fracture site. Interlocking Nail Systems are usually inserted through small “stab” incisions at the end of the bone. This “closed” technique preserves the blood supply and the natural “fracture hematoma” (the collection of cells and growth factors that jumpstart healing), leading to faster recovery times.
2. Early Weight-Bearing and Mobility
One of the greatest enemies of orthopedic recovery is joint stiffness and muscle atrophy caused by prolonged immobilization. Because these nails provide immediate internal stability, many patients can begin physical therapy and even partial weight-bearing within days of surgery.
3. Lower Risk of Infection
By avoiding large open incisions, the risk of post-operative infection is significantly reduced compared to traditional plating methods. The hardware is also protected deep within the bone, further shielding it from external contaminants.
4. Versatility in Complex Fractures
Modern systems are designed with various “locking options.” Some allow for “dynamic” locking, which permits a tiny amount of controlled movement at the fracture site to stimulate bone growth (callus formation), while others provide “static” locking for maximum stability in highly unstable breaks.
The Surgical Procedure: A Brief Overview
The procedure is highly technical and relies on advanced imaging. Surgeons use a “C-arm” (a mobile X-ray machine) to visualize the bone in real-time.
- Reaming: In many cases, the medullary canal is slightly widened using a flexible reamer to ensure a snug fit for the nail.
- Insertion: The nail is guided across the fracture site.
- Locking: Using specialized “jigs” or “targeting devices,” the surgeon precisely places the locking screws through the nail’s holes.
- Verification: Final X-rays ensure the alignment is perfect before the small incisions are closed.
Recovery and Long-Term Outcomes
The recovery timeline varies depending on the severity of the injury, but the use of Interlocking Nail Systems generally facilitates a more predictable path to healing. Within a few weeks, the body begins forming a “callus” or bridge of new bone around the fracture.
In most cases, the nail remains in the bone permanently and does not cause any discomfort. However, if a patient experiences irritation from the screw heads or if the hardware is no longer needed after full union, the system can be removed through a relatively simple outpatient procedure once the bone is completely healed.
Conclusion
The development of Interlocking Nail Systems represents a triumph of engineering in the medical field. By combining the principles of biology and mechanics, these systems allow patients to return to their daily lives faster and with fewer complications than ever before. Whether it is a high-energy trauma from a vehicle accident or a simple fall, modern intramedullary fixation provides the structural foundation necessary for the body to perform its remarkable work of healing.
If you or someone you know is undergoing surgery for a long bone fracture, understanding the role of these interlocking devices can provide confidence in the modern orthopedic approach to recovery.